TMS vs. ECT: Key Differences, Effectiveness, and Safety Compared

Both TMS and ECT are types of brain stimulation therapy that can effectively treat depression. TMS is typically used when you want a more targeted treatment option that builds over time, while ECT is often used when symptoms are more severe and speed matters. Both treatments work, and both have unique advantages. Choosing what treatment is the best next-step in your treatment journey depends on disease type, symptom severity, co-occurring medical conditions, and treatment schedule preference.
If you’ve tried therapy, medication, or both for depression and you’re still not feeling like yourself, it can be frustrating. And when you start weighing options like TMS vs. ECT, it’s easy to feel like you’ve stepped into unfamiliar territory.
The most important thing to know is this: You’re not out of options. You're just moving into a different category of care; one that’s often more targeted, and for many people, more effective.
Transcranial magnetic stimulation (TMS) and electroconvulsive therapy (ECT) are both forms of neuromodulation therapy used to treat depression, especially when other treatments haven’t worked, according to MaryEllen Eller, MD, a psychiatrist at Radial Chattanooga. But they’re not interchangeable.
There is a common sentiment that TMS is "the new ECT" or that it is a "milder" form of ECT. But, those sentiments are false. The treatments differ in how they work, how quickly they act, what they feel like, their side effects, and how much they disrupt your day-to-day life.
It’s also helpful to understand where these treatments fit. For many people, therapy and antidepressants are the first line, and they can work well. But they don’t work for everyone. An antidepressant has only about a 30% chance of leading to remission, and many people still don't respond even with one antidepressant after another. The results for talk therapy are in a similar range. That gap is often what leads people to explore next-step options like TMS and ECT.
If that’s where you are, understanding how these treatments compare can make the decision feel a little more manageable. In this guide, we’ll walk you through the differences between TMS and ECT, plus everything you need to know to better understand what these treatments might mean for you.
What is TMS?
Transcranial magnetic stimulation, or TMS, is a non-invasive brain stimulation therapy that uses magnetic pulses to modify activity levels in the specific brain circuits attributed to disease symptoms.
These network changes contribute to the changes experienced in a depression episode: sleep changes, appetite changes, decreased focus and concentration, mood changes (like tearfulness and irritability), energy chances, decreased ability to experience joy or connectedness. TMS gently targets those areas to help get things working more like they’re supposed to.
Treatment is done in an outpatient setting, like a clinic or doctor’s office. During each session, you sit in a chair while a device delivers a tapping sensation to your scalp. There’s no anesthesia—you’re awake the whole time and can go right back to your normal routine afterward. A typical course of accelerated TMS—the fastest version of the treatment—involves five to 10 sessions per day over five to 10 days, with each session lasting less than 10 minutes.
TMS is most often used for treatment-resistant depression, though it’s also used for conditions such as OCD and is being explored for many other conditions, like anxiety, PTSD, and chronic pain.
Connect with our Clinicians



What is ECT?
ECT is a brain stimulation therapy that sends a brief, controlled electrical current through the scalp to the brain to trigger a controlled, therapeutic seizure. It creates a rapid shift in brain activity and chemistry, which can help reset the network communication patterns involved in mood, often more quickly than other treatments.
It’s done in a hospital setting, under the care of a psychiatrist and anesthesia provider. For each session, you’re put to sleep for a short procedure that lasts just 15 to 70 seconds, so you’re asleep for the procedure and don’t feel anything happening. After that, you wake up in a monitored recovery room. Because of the anesthesia, you’ll need someone to drive you home.
A typical course involves treatments two to three times per week for several weeks, usually totaling around 6–12 sessions. It’s most often used for more severe or urgent cases of depression, especially when other treatments haven’t worked or when faster relief is needed.
How effective are TMS and ECT?
Both TMS and ECT are effective treatments for depression, especially when other approaches haven’t worked, says Eller. And it's important to note that patients must fail pharmaceutical treatment before they'll qualify for insurance coverage, for either of these interventions.
But “effectiveness” isn’t one-size-fits-all. It depends on things like how severe symptoms are, how quickly relief is needed, and how your body responds to treatment.
In general, ECT tends to work more quickly, while TMS is often easier to tolerate and fits more smoothly into daily life. One isn’t universally better than the other—it’s more about which one fits your situation, health needs, and what feels manageable right now. Here’s the breakdown of TMS vs. ECT effectiveness to help you consider which might be the right fit.
TMS effectiveness
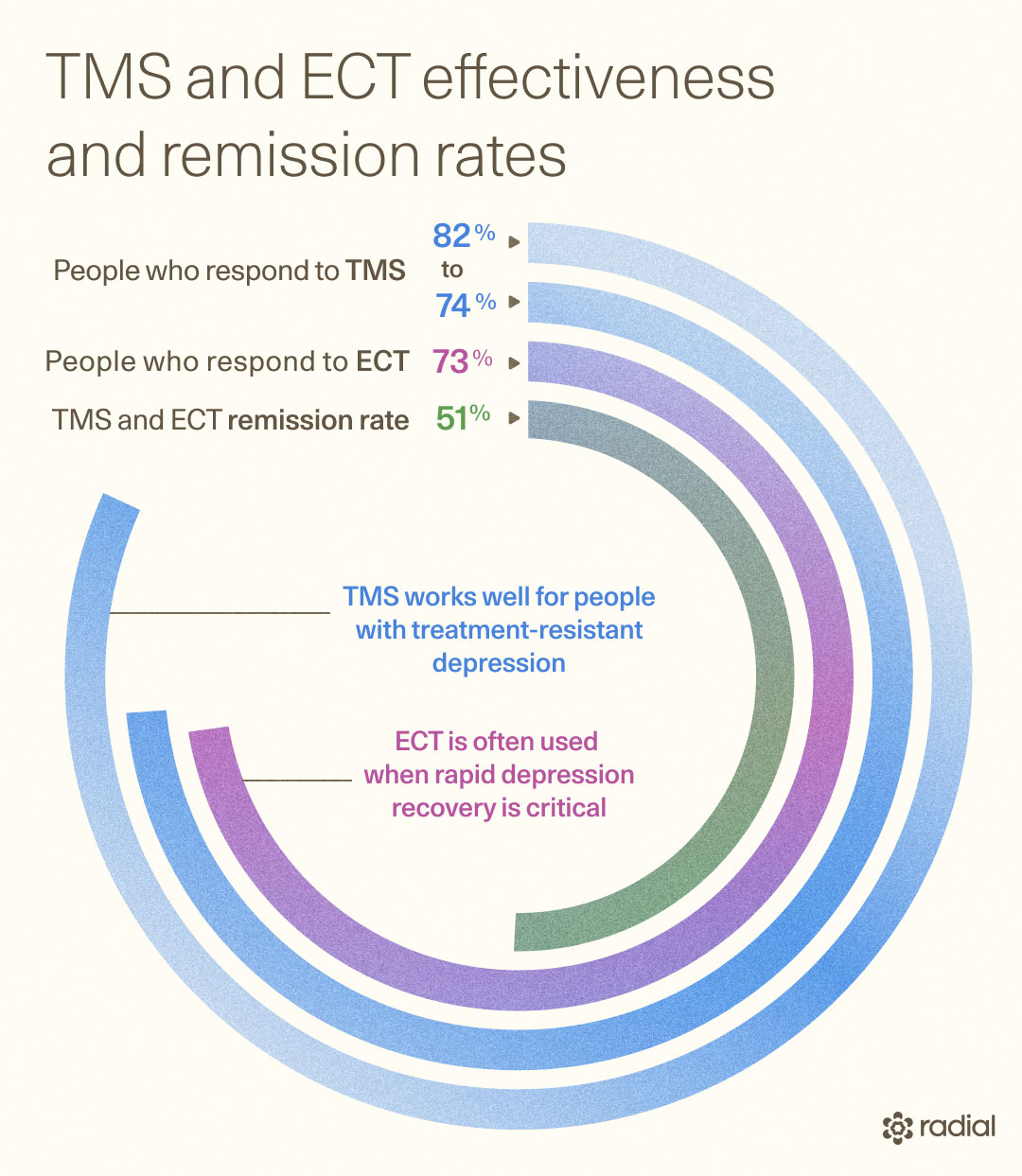
TMS therapy has been shown to work well for people with treatment-resistant depression. Studies suggest that:
- About 74-82% of people respond to TMS (meaning their symptoms improve significantly)
- Around 51% achieve remission (meaning symptoms go away)
- Accelerated TMS protocols have a higher remission rate; SWIFT TMS offers a 78% remission rate and 80% response rate, while SAINT TMS offers a 90% remission rate.
Results don’t happen overnight. Most people notice a difference after a few weeks of consistent treatment, with benefits continuing to build over the full course.
ECT effectiveness
ECT also treats severe depression. It’s often used when rapid depression recovery is critical; for instance, in the case of suicidal thoughts, psychosis, catatonia, or severe functional impairment.
Research shows that:
- About 73% of people respond to ECT
- About 51% achieve remission
Unlike TMS, which builds gradually, ECT often works more quickly. Some people begin to notice meaningful improvement within days to weeks, which is part of why it’s used when you need to get rid of depression symptoms fast.
Another important difference is that ECT is sometimes the best treatment for conditions that TMS isn’t used for at all. For example, ECT can work very well for depression with psychosis or catatonia. ECT is also an effective option for bipolar disorder and schizophrenia, where TMS is still relatively unproven.
What are the side effects of TMS vs. ECT?
If you’re curious about the potential side effects of each treatment, you’re not alone. This is often one of the biggest considerations.
Both TMS and ECT are considered safe and well-studied treatments, but they come with different types of risks and tradeoffs. And understanding what those might feel like can help you go in with clearer expectations.
TMS side effects
TMS is generally well-tolerated. And for most people, side effects are mild and tend to ease as treatment goes on.
Some people notice scalp discomfort, especially early in treatment. It can feel like tapping or sensitivity at the treatment site, but it usually improves over time. Others may experience a mild, short-lived headache, which can often be managed with over-the-counter pain relievers.
During the session, you might notice some facial twitching due to nerve stimulation, but this stops as soon as the treatment ends. Some people also feel briefly lightheaded. In very rare cases, a seizure can occur.
ECT side effects
ECT is also considered safe. But because it involves general anesthesia and a controlled seizure, the side effects can feel more noticeable—and it’s totally normal to have questions about what to expect.
Some people experience memory changes, like having trouble recalling recent events or forming new memories during treatment. For many, these effects are temporary, though in some cases there can be longer-lasting gaps.
It’s also common to feel a bit confused right after a session, especially as you’re waking up from general anesthesia. This can feel unsettling in the moment, but rest assured that it usually clears within minutes to hours.
Other side effects can include headaches or mild muscle soreness after treatment, along with nausea or grogginess from the anesthesia.
For many people, these side effects are manageable, especially when you weigh them against the potential benefits of treatment and the risk of under-treated or untreated mental illness. And if you’re considering ECT, your care team will walk you through what to expect at every step so you’re never left guessing.
What TMS and ECT actually feel like
A lot of people get to this point and think: Okay, but what is this actually going to feel like?
That’s a fair question. These treatments can sound intimidating on paper, but the lived experience is often much more straightforward—and less scary—than you’d expect.
What a TMS session is like
TMS is designed to feel pretty low-key.
At your first visit, your provider will map your brain to find the exact spot to target. They do this by delivering a few test pulses and observing small responses—like a brief movement in your hand or foot—to calibrate the right location and intensity for your treatment.
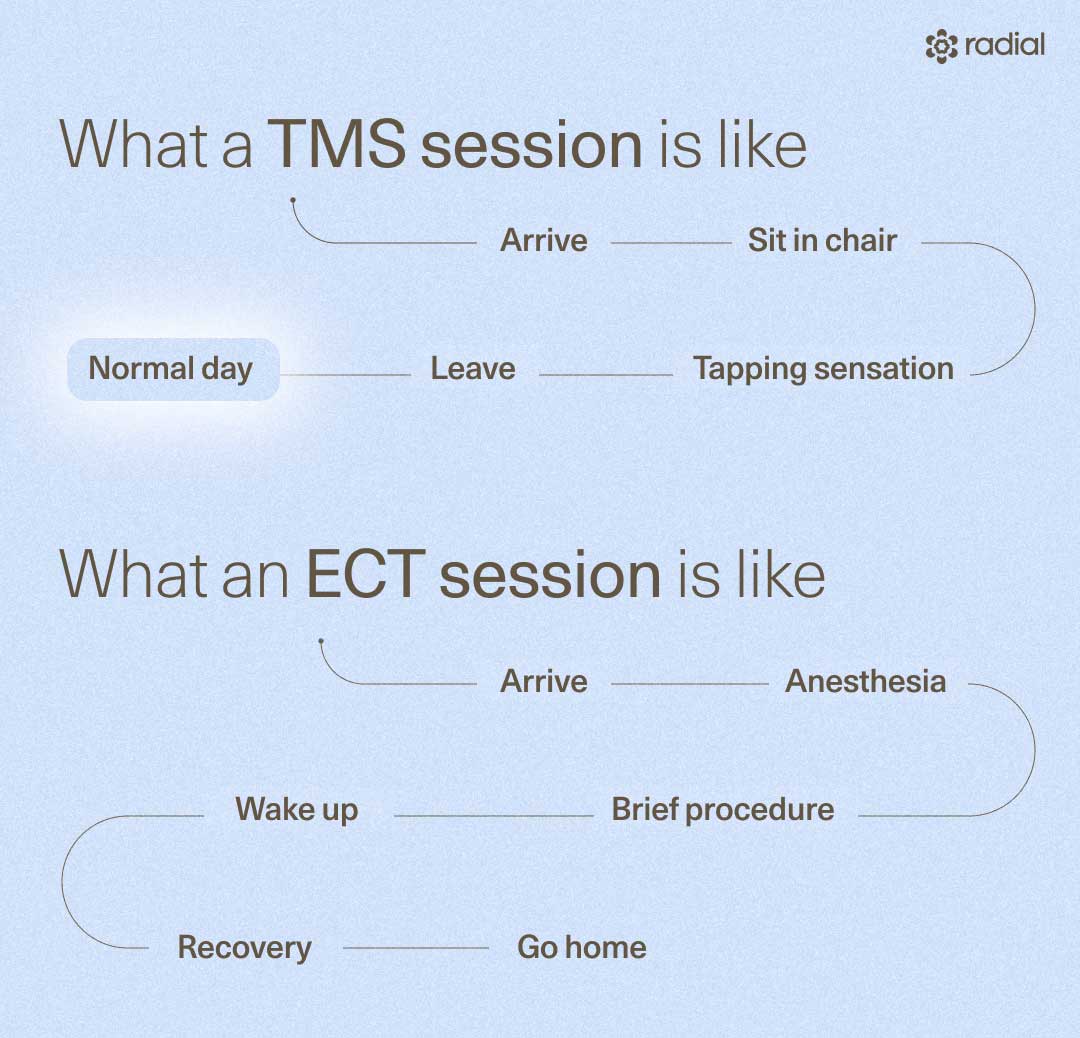
After that, sessions tend to follow a simple, predictable routine:
- You’ll sit in a comfortable chair while a device rests against your scalp.
- You’ll feel a tapping sensation once the treatment starts. It’s often described as a light knocking or steady, rhythmic pulse.
- You’ll stay awake for the full session, and can talk to the technician, or just zone out.
If you’re considering TMS, it’s also natural to wonder what it actually feels like. For most people, it feels more uncomfortable than painful, and that initial sensitivity often fades after the first few sessions.
After each session, you can walk out, drive home, and go about your day. There’s no recovery time, which is why it tends to feel more like a regular appointment than a medical procedure.
What an ECT session is like
ECT is a more involved experience, but it’s also much more controlled and supportive than people often imagine. Here’s what it usually looks like:
- You’ll arrive at a hospital or treatment center, where the care team will walk you through the process and get you set up for the procedure.
- You’ll rest in a hospital bed while a nurse places your IV line and connects you to monitors (EKG, O2, EEG)
- You’ll be given general anesthesia through an IV, so you’ll be asleep before anything begins.Through the IV, you'll get one medicine to make sure that you're asleep, and another medicine to relax your muscles during the seizure."
- While you’re fully asleep and relaxed the psychiatrist will deliver a brief electrical stimulus inducing a brief, controlled seizure (lasting 15-70 secs). It is the seizure that is thought to be what makes patients better, not the electricity itself.
- You’ll wake up in a supervised recovery area after about 10 minutes, often feeling groggy or a bit disoriented at first.
- You’ll remain in the recovery area for at least 30 minutes while the effects of general anesthesia wear off.
- You’ll need someone to drive you home, and most people plan to take it easy for the rest of the day.
Some people worry that ECT might change who they are. That’s an understandable concern. But know that ECT is designed to treat symptoms of severe mental illness, not change your personality.
ECT can also feel like a bigger medical procedure compared to TMS. It includes general anesthesia, the procedure itself, and recovery time afterward. Most people feel groggy when they wake up and need to take the rest of the day off. You're also not allowed to operate a motor vehicle within 24 hours of receiving general anesthesia.
It’s normal for ECT to feel like a big step, and your care team will be there to support you through every part of the experience.
TMS vs. ECT: How doctors decide which treatment to use
When doctors are helping you weigh TMS vs. ECT, they’re looking at the full picture: how severe your symptoms are, how quickly you need relief, what you’ve already tried, what additional medical conditions you're managing, and what’s actually realistic for your day-to-day life.
TMS may be recommended if:
TMS is FDA-cleared to treat major depressive disorder, OCD, migraines, and for smoking cessation. It may also be a good fit if:
- Symptoms haven’t improved with medication
- You want a lower-disruption option that fits into your routine
- You prefer to avoid anesthesia or memory-related side effects
- You can commit to frequent outpatient sessions
Note: FDA clearance and insurance coverage are not the same. Check your insurance company’s eligibility criteria to learn more about coverage.
ECT may be recommended if:
ECT is FDA-approved to treat severe and treatment-resistant major depressive disorder, bipolar disorder, and catatonia. In practice, that means it may be worth considering if:
- Symptoms are severe, worsening, or urgent
- You’re experiencing suicidal thoughts or psychosis
- Other treatments haven’t worked
- Faster relief is needed
Remember: You don’t have to figure this out alone. A Radial specialist can help you weigh the tradeoffs and choose the option that works best for you.
The pros and cons of TMS vs. ECT
By this point, you might be trying to weigh what ECT vs. TMS would actually mean for you—not only how they work, but how they’d fit into your life.
There’s no perfect option here. Both TMS and ECT can be effective, but they come with different tradeoffs in terms of time, intensity, side effects, and day-to-day impact. Here’s a simple way to think through those differences:
Pros and cons of TMS
Pros:
- Non-invasive—no anesthesia required
- No recovery time
- Minimal cognitive side effects (does not disrupt memory consolidations)
- Fits more easily into daily life
- Effective for many people with treatment-resistant depression
- Able to drive yourself to/from the clinic for treatment
Cons:
- Requires frequent sessions over several weeks
- Results build over weeks
- Not as fast-acting for severe or urgent symptoms
- May not be sufficient for more complex or severe cases
Pros and cons of ECT
Pros:
- To date, the most effective treatment for severe depression
- Works faster than most other options
- Especially helpful in urgent or complex cases
- Can be effective when many other treatments haven’t worked
Cons:
- Requires general anesthesia and a medical procedure setting
- Temporary memory issues and confusion are common
- Requires recovery time after each session
- Greater disruption to daily routine
- More logistical coordination (transportation, time off, etc.)
In some cases, “these modalities [are] not recommended due to substantial time and scheduling constraints that would interfere with the patient’s ability to maintain employment,” adds Eller.

Cost and insurance considerations
Cost is a real part of this decision, and it’s completely normal to have questions about it.
Both TMS and ECT can be covered by insurance, especially for FDA-approved uses like treatment-resistant depression. But the details can vary depending on your plan. In many cases, insurance will want to see that you’ve tried other treatments first and that your symptoms are severe enough to meet their coverage criteria.
The experience can also look a little different between the two. TMS is done in an outpatient setting, so coverage is usually tied to office visits and repeated sessions over time. ECT, on the other hand, involves general anesthesia and occurs in a hospital setting. That means it’s often billed more like a medical procedure, with additional charges like facility and anesthesia fees.
Across both treatments, out-of-pocket costs and insurance requirements are some of the most common challenges people run into. The upside is that your care team can help you navigate all of this, so you’re not figuring it out on your own.
Relief within reach
Care covered by your insurance
Radial provides advanced mental health treatment, covered by the insurance you already use.








The bottom line
If you’re comparing TMS vs. ECT for depression, the good news is that both of these treatments can help. ECT tends to work faster and is often used in more severe or urgent situations, while TMS is less disruptive and builds more gradually over time. Neither is “better” than the other—it’s about what fits your symptoms, timeline, and life.
You don’t have to figure this out on your own. A Radial specialist can help you weigh the options and guide you toward the right fit. And if your symptoms are getting worse, not improving, or starting to feel urgent, that’s a sign to reach out. There are more options than you may realize, and you don’t have to navigate them alone.
Key takeaways
- TMS and ECT are both effective treatments for depression, especially when other options haven’t worked.
- TMS is non-invasive, lower-disruption, and builds results gradually over several weeks.
- ECT works faster and is often used for more severe or urgent symptoms.
- The right choice depends on your symptoms, treatment history, and how each option fits into your life.
- You don’t have to make this decision alone—working with a Radial specialist can help you find the best path forward.
Frequently asked questions (FAQs)
Does ECT cause permanent memory loss?
It is important to note that while temporary memory issues are common, they're not guaranteed. In fact, about 30% of people actually demonstrate improved memory scores during ECT treatment. Many factors influence your brain's ability to remember information: ECT is one of them. Under-treated/un-treated mental illness also has severe and long-lasting impacts on memory.
How long does TMS take to work?
TMS doesn’t work overnight. Most people start to notice changes after a few weeks of consistent treatment, with benefits continuing to build over the full course (usually four to six weeks).
Is TMS safer than ECT?
Both treatments are considered safe. TMS is less invasive and doesn’t require general anesthesia, so it has fewer risks and side effects overall. ECT is also safe when performed under medical supervision, but it involves anesthesia and can cause temporary memory issues, which some people want to avoid.
Deep dive recommendations
- The TMS Podcast.
- Inside Bipolar Podcast. Psych Central. ECT: Medical torture or effective treatment? (Electroconvulsive therapy).
- The Frontier Psychiatrists. Magnetic fields, magic, and mental health.
- Psychiatry & Psychotherapy Podcast. Episode 152: ECT efficacy and controversies with Dr. Cummings.
- Psychiatry & Psychotherapy Podcast. Episode 201: Psychotic depression with Dr. Cummings.
- Psychiatry & Psychotherapy Podcast. Episode 73: Catatonia: Diagnosis and treatment.
Editorial Standards
At Radial, we believe better health starts with trusted information. Our mission is to empower readers with accurate, accessible, and compassionate content rooted in evidence-based research and reviewed by qualified medical professionals. We’re committed to ensuring the quality and trustworthiness of our content and editorial process–and providing information that is up-to-date, accurate, and relies on evidence-based research and peer-reviewed journals. Learn more about our editorial process.
Let's connect
Get started with finding the right treatment for you or someone you care about
Get started




